
Finding my Voice in the Delivery Room:
The moment I first held my baby should have been pure joy. Don’t get me wrong, It absolutely was, but it was clouded by the fog of surgical recovery and the lingering question: “What just happened to me?”
My first birth experience left me traumatized, both physically and emotionally. I was confined to a hospital bed for nearly 24 hours, denied the ability to move freely, and ultimately wheeled into an “emergency” C-section that may have been avoided — I came out from this experience not just with a beautiful baby, but with a body that couldn’t walk for weeks and a mind full of doubt.
What I didn’t realize then was how that one birth outcome — would cast a shadow over every future pregnancy. In the birthing world, once you have a C-section, you’re often automatically pushed toward repeat surgeries, regardless of your desires or circumstances.
But this isn’t just my story of trauma. It’s about what happened next — how I discovered options I never knew existed, educated myself beyond what most providers share, and reclaimed my power in the delivery room for my subsequent births. It’s about the contrast between my first traumatic surgical birth and my later empowering, natural VBAC deliveries.
I’m sharing my journey because what I’ve learned could save you from unnecessary trauma, and from the struggle of fighting against a system that operates from the base of the risk control rather than supporting the natural birth process. My story shows that with the right preparation, knowledge, and support, you can find your voice in the delivery room and experience birth on your own terms — even when the medical system might try to convince you otherwise.
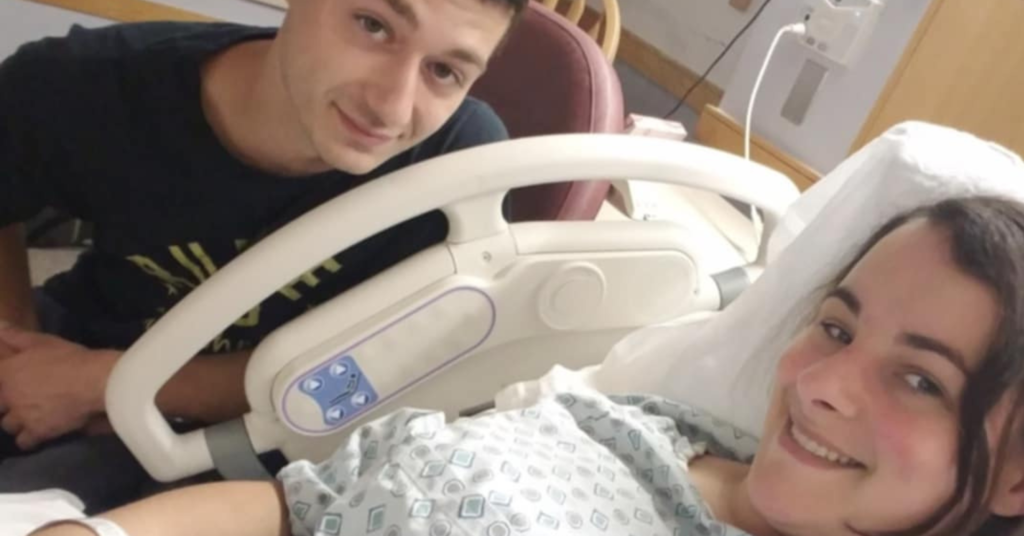
My First Birth: When Lack of Preparation Led to Trauma
Looking back, I entered my first birth with hope but without preparation. Like many first-time moms, I had an ideal scenario in my head — a natural, non-medicated birth — but no real strategy for achieving it. I trusted the system completely. After all, the doctor knows best, right?
When my water broke and labor began, I headed to the hospital with excitement. But that excitement quickly faded as I was told I need to stay in bed, hooked up to monitors, and unable to move freely. I felt like it was necessary for me to stay still, so my team could monitor my baby. No one told me I could advocate for mobility during labor. No one explained how movement could help progress things naturally. At 5cm dilated, I was essentially immobilized for what would become a grueling 24-hour ordeal.
The cascade of interventions began:
- Restricted to bed rest
- Limited positions for laboring
- Epidural (which I requested when pain became unberrable)
- Slowed labor progression (Thanks epidural)
- Pitocin administration ( Let’s speed things up)
- Epidural turned off while Pitocin increased (so I knew when to push and so they could tell when I’m contracting)
Oh let me tell you, my body didn’t like this idea at all — vomiting, shaking, and emotional distress took over. After allowing me just three practice pushes, my obstetrician declared an “emergency C-section” necessary, citing the 24-hour timeframe since my water broke.
In that moment of vulnerability and fear, I didn’t question. I didn’t ask:
- “Is this truly an emergency?”
- “What are my alternatives?”
- “Can we try different positions for pushing?”
- “What are the risks versus benefits?”
I simply nodded, terrified and trusting that this was the only option. It wasn’t until much later that I began to wonder if things could have gone differently.
The surgery itself felt impersonal and clinical. The joy of meeting my baby was overshadowed by the bright lights, the surgical team’s casual conversation, and the bizarre sensation of pressure without pain as they operated.
What I didn’t understand then — what no one explained to me — was that this single decision would have implications for every future pregnancy. That by accepting this C-section which is a major abdominal surgery without question, I was unknowingly setting myself up for a battle to reclaim my birth autonomy and fight for VBAC opportunities for years to come.

The Aftermath: Recovery and Realization
The hours and days following my C-section were a harsh awakening to the reality of surgical birth recovery. The pain was debilitating. What should have been a time of bonding with my newborn became a struggle to perform basic self-care while managing excruciating pain.
For weeks, I couldn’t move normally. The incision burned, my abdomen felt weak, and the simplest tasks required assistance. This wasn’t just about physical discomfort—it was about a profound loss of independence during this time when I needed my strength the most.
During those long recovery days, questions began haunting me:
- What if I had been allowed to move during labor?
- What if I’d had someone to advocate for me when I was too exhausted to do so myself?
- What if I had prepared differently, known more, asked better questions?
- Was that C-section truly necessary, or was it a result of hospital protocols and convenience?
These questions took on greater weight when my husband and I discussed our family plans. We had always dreamed of having several children, but now a shadow loomed over that vision. I began researching repeat C-sections and discovered concerning facts about increasing risks with each subsequent surgery:
- Higher chances of placenta complications
- Increased risk of surgical adhesions
- More difficult recoveries
- Greater likelihood of NICU stays for babies
The medical providers message seemed clear: once you have a C-section, you’re destined for surgical births thereafter. This felt like a life sentence—one that would limit not just how I gave birth, but potentially how many children we could safely have.
The realization that one unprepared time had possibly altered my entire reproductive future was devastating. I felt robbed of choices I didn’t even know I needed to protect.
Discovering VBAC: There Were Options After All
The turning point came unexpectedly. During a casual conversation, a friend mentioned her “amazing OBGYN, Dr. Lovier who performs VBACs at MVHS.” Those words—vaginal birth after cesarean—stopped me in my tracks. I had no idea this was even a thing.
It was as if someone had opened a door I didn’t know existed. The medical narrative I’d accepted—that my body was somehow permanently altered, requiring surgical births forever—was being challenged.
I jumped into VBAC research with newfound determination:
- I learned that VBAC success rates range from 60-80% for most women
- I discovered that the much-feared uterine rupture risk is actually less than 1%
- I read countless stories of women who had successful, empowering VBACs
- I found studies showing that recovery from vaginal birth is typically faster and less complicated
The statistics were eye-opening. We have more risk dying in car accident than from complications during vaginal birth after a C-section—yet we don’t tell people they can’t drive. Meanwhile, many doctors use fear tactics to push women toward repeat surgeries that carry their own significant risks.
Armed with this knowledge, I sought out Dr. John Lovier, the VBAC-friendly provider my friend had mentioned. The difference was immediate and profound. Instead of dictating my care, this doctor:
- Asked about my birth goals
- Explained all options with balanced information
- Acknowledged the low statistical risk of VBAC complications
- Expressed commitment to supporting my decisions
- Treated me as a partner in my own care, not just a patient
“I’m here for you and what you want in your birth and pregnancy,” Dr. Lovier told me. “I’ll do everything I can for you to reach those goals.” After feeling like a passive participant in my first birth, these words were revolutionary. For the first time, I felt seen as a person with agency over my own body.
The discovery that I had options—that my birth story wasn’t predetermined by my surgical past—ignited something in me. I wasn’t just hoping for a better experience this time; I was determined to create it through knowledge, preparation, and the right support.
Preparation Makes All the Difference
With my second pregnancy, I approached birth differently. This time, I wasn’t leaving anything to chance. I realized that knowledge and preparation would be my greatest tools in achieving the birth experience I desired.
My preparation became a full-time commitment:
I immersed myself in education:
- Studied natural pain management techniques
- Researched optimal positions for labor progression
- Learned about the physiological stages of birth
- Watched positive VBAC birth stories
I prepared my body:
- Regular chiropractic adjustments to optimize pelvic alignment
- Focus on nutrition to support recovery and strength
- Walking and movement to build stamina
I built a support system:
- Joined a VBAC support group on Facebook
- Connected with other mothers who had successful VBACs
- Developed relationships with supportive medical providers
I created a detailed birth plan.
This level of preparation wasn’t just about increasing my chances of a vaginal birth—it was about reclaiming my power in the birthing room.
The first time, I had walked into the hospital hoping for the best but willing to defer to others’ judgment. The 2nd time, I was walking in as an informed advocate for myself and my baby, with clear goals and the knowledge to pursue them.
What I didn’t expect was how this preparation would transform not just my birth experience, but my sense of self. The woman researching VBAC statistics late into the night was discovering a strength and determination she hadn’t known before. I found the power in myself that wasn’t there the first time around.

My Second Birth: A Redemptive VBAC Experience
When I developed preeclampsia at 37 weeks with my second baby, I knew my birth would require some medical intervention. But unlike my first experience, I faced this induction with confidence and clear boundaries.
I remember the first question to Dr. Lovier upon arrival to the hospital: “How long until you make me have a C-section?” His answer changed everything. He looked me in the eyes and said, “I would never make you have a C-section unless there was an emergency where the baby or you were at risk”
The relief was huge. No random timeline. No rushing the process. No “failure to progress” diagnosis after some hospital-determined deadline. This single statement created a foundation of trust that would support me throughout labor.
Despite needing an induction for medical reasons and birthing in the same hospital (St. Lukes), I was determined to labor as naturally as possible. This time was different:
- I moved freely, changing positions frequently
- I used the birthing ball to ease discomfort
- I stood, squatted, and walked when I needed to
- I used breathing techniques I had practiced
- I worked with my body’s rhythms rather than fighting them
The hospital staff respected my VBAC birth plan, offering support without pushing interventions. When contractions intensified, I relied on the techniques I had practiced rather than immediately requesting medication. My body was doing exactly what it was designed to do, and I was allowing it to lead the way to a successful VBAC.
Perhaps most telling was the pushing phase. Unlike my first birth, where I was given three “practice pushes” before being rushed to surgery, this time no one coached my pushing. I simply listened to my body’s cues and pushed when I felt the urge. That same monitoring and tracking of contractions that my first doctor insisted was crucial for pushing? Turns out it wasn’t needed after all.
The moment my baby was born naturally changed everything. I felt the sense of accomplishment and empowerment. I had done it—a successful, non-medicated VBAC that many would have said was impossible.
But the differences didn’t end with delivery. The recovery was night and day compared to my surgical birth. Within an hour, I was up walking around, feeling almost normal with minimal pain. No catheter. No incision care. No pain medications. Just my body, already beginning to heal itself as nature intended.
This experience confirmed what I had suspected after my C-section: there had been another way. My body hadn’t failed me the first time—the system had failed to support my body’s natural abilities.
With this redemptive experience, I knew beyond doubt that any future children would deserve the same informed, empowered approach. What I didn’t yet realize was that even with this success, I would face new obstacles in my birth journey.
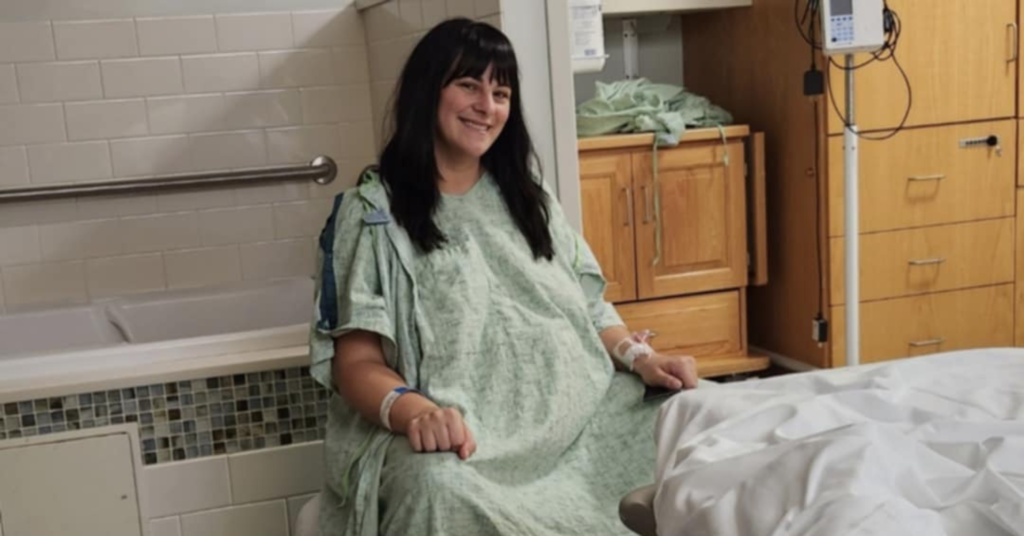
The Hidden Challenges: Hospital Policies Matter for VBAC
My journey to a third birth revealed another rarely discussed obstacle: hospital policies can override provider support. Despite working with the same VBAC-friendly doctor who believed in my body’s capabilities, I learned the hospital he practiced at the time (Rome Health) didn’t permit VBACs—a policy completely disconnected from my personal history and proven ability to deliver vaginally.
This unexpected roadblock forced me to make difficult decisions late in my pregnancy:
- Switch providers in my third trimester
- Travel an hour from home to receive care and deliver at VBAC friendly Bassett Healthcare
- Navigate an unfamiliar healthcare system
- Build trust with new providers quickly when I was most vulnerable
The realization was both frustrating and eye-opening. Why should rigid hospital policy dictate my birth options when I’d already proven my body could safely deliver vaginally after a cesarean? The answer often comes down to institutional risk management rather than individualized care. Most often it comes down to 24/7 Anesthesia coverage that some hospitals don’t have.
Birth choices shouldn’t require such extreme efforts, yet many women face similar barriers every day.

My Third Delivery: Continued VBAC Success
Armed with my previous experience and hard-won knowledge, my third birth proceeded with a confidence I couldn’t have imagined during my first pregnancy. I applied the same principles that had served me well before:
- Clear communication of my birth plan with all providers
- Confidence in advocating for my needs when necessary
- Deep trust in my body’s natural abilities and wisdom
Despite the provider and location changes, the result was another beautiful, non-medicated VBAC with no interventions. My body led the process with the medical team providing support without unnecessary interruptions.
With each successful natural birth, my confidence grew, further validating my suspicion that the initial C-section likely hadn’t been necessary in the first place.
The Lasting Impact: Still Fighting for VBAC Birth Rights
Could you believe that six years and three pregnancies later, that first C-section continues to affect my care? Now pregnant with my fourth child, I have been told I need to have a C-section to deliver at certain hospitals despite two successful vaginal births that proved my body’s capabilities. Thankfully, I know better now and know how to advocate for what’s nonnegotiable.
The medical system’s memory is long when it comes to surgical births, but curiously selective when it comes to successful VBACs. That single C-section—possibly unnecessary and certainly performed without exhausting all options—still determines how providers and healthcare systems view my body and delivery risks, regardless of subsequent evidence to the contrary.
This shows why avoiding that first unnecessary C-section is so important for women who desire multiple children. It’s not just about one birth experience—it’s about preserving choices for your entire reproductive future.
Key Takeaways for Expectant Mothers

After three births and years of research, these are the essential lessons I’ve learned:
Knowledge truly is power in the birthing room.
- Understanding the physiological process of birth helps you recognize normal versus concerning developments
- Knowing the latest evidence-based recommendations gives you confidence when questioning interventions
- Being informed about your rights as a patient allows you to set boundaries effectively
Provider selection is more critical than most realize.
- Interview multiple providers before committing
- Ask direct questions about their C-section rates and VBAC support
- Listen for language that respects your autonomy versus dictates your care
- Trust your instincts about how they respond to your questions
- Don’t be afraid to switch if you feel uneasy
Hospital policies can override provider promises.
- Research facility statistics and policies separately from your provider
- Ask about specific protocols for VBAC, labor time limits, and movement during labor
- Consider birth centers or hospitals with lower intervention rates
Your voice matters most in your birth experience.
Preparing responses to common pressure tactics gives you confidence in the moment
No one can make you consent to procedures you don’t want
You have the right to ask questions before agreeing to interventions
Bringing a dedicated advocate (partner, doula, friend) helps when you’re vulnerable
Achieving the Empowered Birth you Wished for
Don’t walk into your birth unprepared as I did with my first child. Take action now to ensure you have the knowledge, confidence, and support to create the birth experience you deserve.
You can start by downloading these free resources which helps expecting mothers prepare here

Then look for prenatal education and birth preparation classes near you such as 6 week Empowered Birth and Beyond workshop offered by Mohawk Valley Lactation.
This program covers everything I had to learn the hard way:
- Evidence-based information about birth options
- Effective advocacy strategies for the hospital setting
- Natural comfort measures for labor
- Partner support techniques
- Postpartum preparation
- Community with other expectant parents
Check out and register for it here. to secure your spot and take the first step toward an empowered birth experience that honors your body’s wisdom and preserves your future choices. Your baby’s birth day is too important to leave to chance.


0 Comments